Combining an Authentic4D MRI Review with an EMG Review
Close claims faster and avoid unnecessary expenses
MRI (Magnetic Resonance Imaging) and EMG (Electromyography) are diagnostic tests that help clinicians assess and pinpoint medical issues. Often times an MRI is followed by an EMG when clinicians are working to understand, diagnose, and ultimately treat a patient. MRI and EMG reports tend to “complement” one another and allows for a more comprehensive depiction of the patient’s medical condition. This means that an MRI and an EMG will generally reach the same conclusion regarding pathology even though they are based on very different technology. Certain inconsistencies between the results can be an indication of inaccurate exam results.
Authentic4D’s MRI reviews are extremely compelling all on their own but when combined with an EMG review, the result can be like a missing puzzle piece that offers powerful evidence and is tremendously impactful when defending your position.
Being able to reference the A4D written imaging report provides our EMG experts puzzle pieces to definitively opine that there is no mechanical evidence of a radiculopathy at a certain level. This allows the claims professional to refute the claim and improve patient care and outcomes.
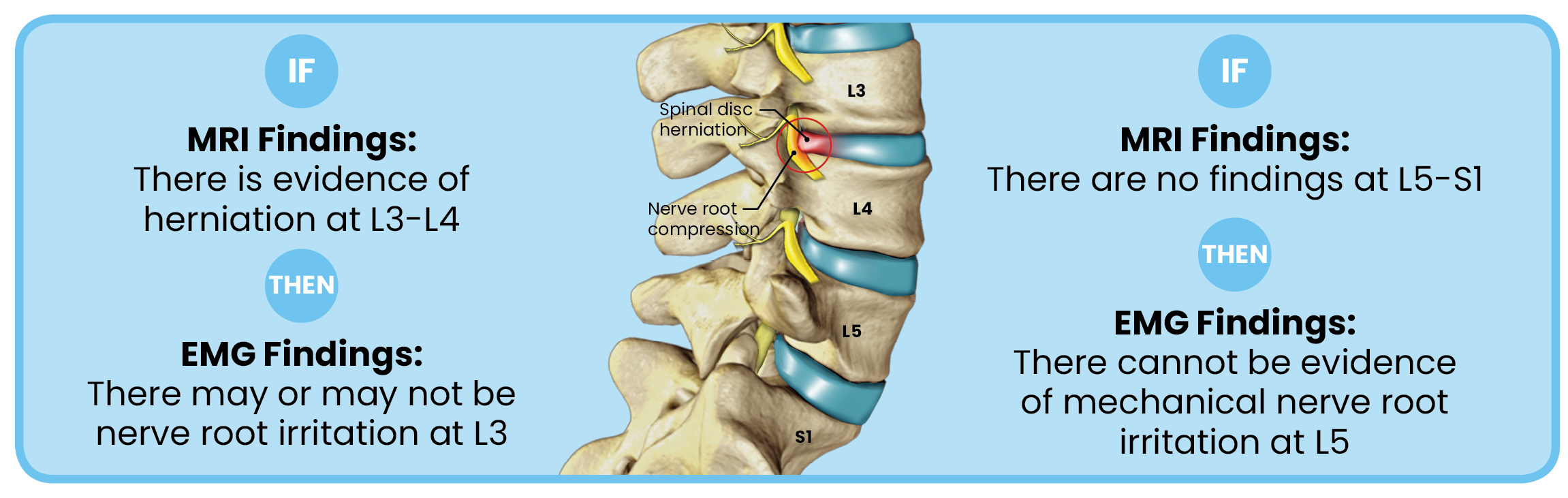
A disc bulge at L3-L4 on an MRI can have EMG findings indicative of nerve irritation or damage or no EMG findings at L3 (an asymptomatic patient). If there is no finding on the MRI at L5-S1 level, the EMG cannot indicate that there is a mechanical radiculopathy at the L5 nerve root.
If an A4D sub-specialized radiologist said there were chronic degenerative changes at L3-L4 but no findings at L5-S1 and the original EMG report said there was evidence of radiculopathy at L5-S1, you know that the EMG was:

Value in both
Whether we agree or disagree with the original imaging report, a written report by A4D’s sub-specialized radiologists complements EMG reports in a way that adds immense value to a case. Here are two specific examples of how beneficial the MRI and EMG reviews are when done in conjunction with one another:
Clinical Use Case – A4D “Disagree” Example:
Claimant Vickie Smith states she has arm and neck pain after being rear ended. She had a cervical spine MRI for these complaints and a few days later she had an EMG. The claims professional requested that Authentic4D complete an MRI review of Vickie Smith’s original MRI findings.
The original MRI report said there were acute changes at C3-C4 and C4-C5. Upon review by A4D’s sub-specialized radiologists, only chronic findings were found at C4-C5 and C5-C6. This was noted in the A4D written report.
The original EMG report diagnosed radiculopathy at C3 and C4 as a result of the accident. Upon review, our EMG expert had suspicions on the quality of this diagnosis based on medically improbable values in the report and disagreed with the findings.
The ability to review his EMG findings side-by-side along with the A4D imaging report allowed the conclusion to become even more clear: The MRI was over-reaching and the EMG cited findings that were nonexistent.
Clinical Use Case – A4D “Agree” Example:
Claimant Luke Jones has low back pain from a slip and fall. His MRI showed an acute herniation at L5-S1 on the original imaging and no other changes. The claims professional submitted Mr. Jones’ original MRI to Authentic4D for review. A4D’s radiologist agreed with the acute finding at L5-S1.
Upon review of the original EMG, our expert noted inconsistencies in the data and questioned the diagnosis of L3 radiculopathy. He compared the EMG findings to the imaging report and reached the conclusion that the MRI was medically useful, but the EMG was of poor quality and could do more harm than good if used for patient care.
Quality physicians, quality outcomes, and the missing puzzle piece
High-quality clinicians are critical to optimal patient outcomes. Authentic4D’s clinicians have the highest level of education and training. They go through a rigorous vetting process and their work is reviewed continuously (not just their credentials). Our sub-specialized radiologists read studies blindly and have zero incentive to tell others what they want to hear.
Finally, it is extremely important to view MRI and EMG findings as pieces to the same puzzle. Each diagnostic test can provide clues that ultimately give the claims professional a comprehensive understanding of the claimant’s medical condition. When the “medical puzzle” is complete, outcomes are exponentially improved.
Request More EMG Information
Take the next step
Request a Demo
A knowledgeable member of our team will be in touch to find a convenient time to demonstrate our solution.
Submit a Case
Ready to try Authentic4D? Submit your claim file to get an evaluation within 48 hours.
Explore
Seekers of Truth
About Us
Search
Copyright © 2022 Authentic4D. All rights reserved.
